0 Comments
According to CNN news, since the outbreak of COVID-19, a condition called “broken heart syndrome” significantly increases.
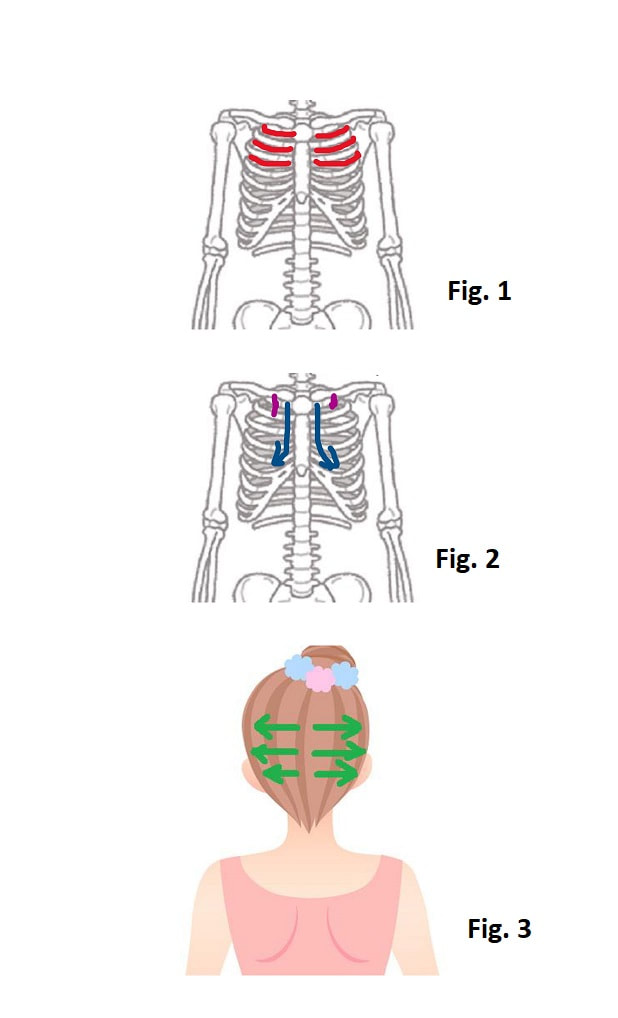
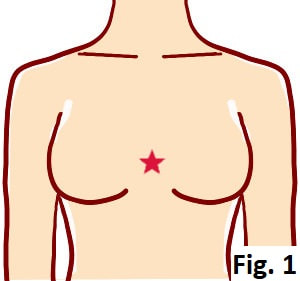
Broken heart syndrome is a temporary heart condition that's often brought on by stressful situations and extreme emotions. The condition can also be triggered by a serious physical illness or surgery. Broken heart syndrome symptoms can mimic a heart attack. Common symptoms include: Chest pain Shortness of breath I want to introduce a self-care method for this condition. If they are caused by stressful situations due to COVID-19, the following self-care can treat the condition, which is introduced by Mr. Niki, an acupuncturist in Japan. 1. Find a tender point on the bone in the center of the chest at the level of your nipples, which is an acupuncture point CV-17 (Fig. 1). 2. Touch the tender point with the edge of a penny gently (Don’t press it hard into the skin) (Fig. 2). 3. Hold the penny for 5 seconds. After doing this, instantly you could feel that your chest opens or you feel relaxed, and you could breathe deeply. Whenever you feel stressed or can’t breathe deeply, please try this method. What you need is just a penny! CNN news article for reference Aspiration Pneumonia
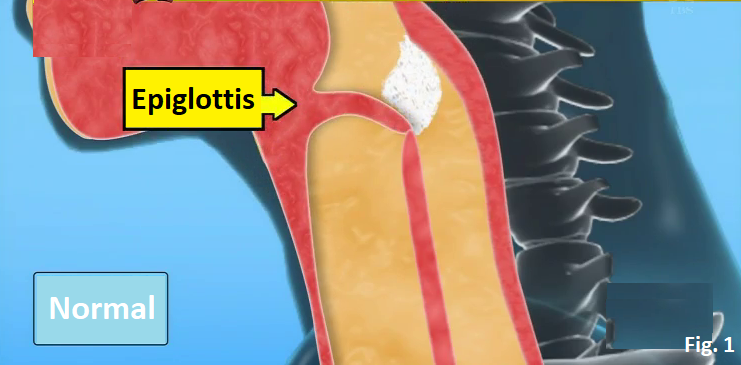
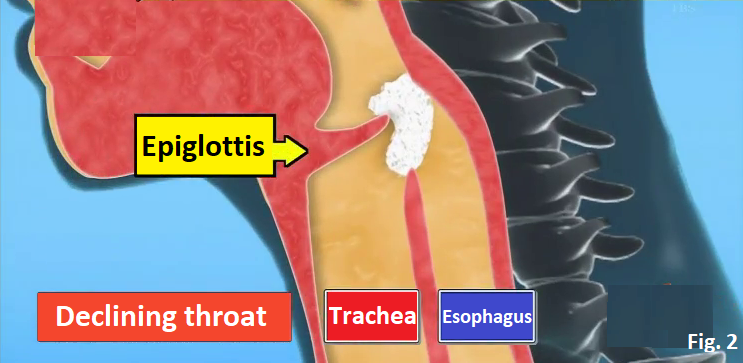
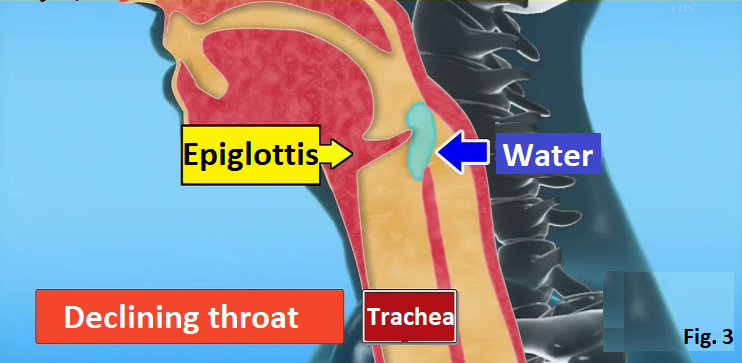
People who choke on something to eat have high risk of developing aspiration pneumonia. How does aspiration pneumonia occur? In the case of normal people, the epiglottis (the flap covering the trachea) in the throat closes when eating food so that the food is delivered to the esophagus (Fig. 1). But in the case of people whose function of the throat declines with age, the epiglottis in the throat doesn’t close well so that the food enters the trachea. As a result, bacteria propagate from the food delivered to the lung, causing pneumonia (Fig. 2). It is supposed to be impossible to know whether the function of the throat declines or not without X-ray at the hospital. But by drinking a glass of water, you can check whether the function of your throat declines or not. How to check the decline of your throat Drink up 100 cc (3.38 FL OZ) of water within 10 seconds. If you can’t drink up within 10 seconds or if you choke in the middle of drinking it, there is a high possibility that the function of your throat declines. Since people with the declining throat like the elderly can’t close the epiglottis, they choke and can’t drink water well when they drink it at a gulp (Fig. 3). The elderly tends to drink tea or coffee little by little, so it is difficult to notice that the function of their throat declines. How to strengthen the function of the throat Lift-Up-Jaw exercise: (1) Place the fists of both hands under the jaw (Fig. 4). (2) Push your jaw to your fists and keep pushing each other for 5 seconds (saying “Eeh” while doing this is more effective) (Fig. 5). (3) Repeat (1) and (2) for 10 reps. (4) Do (3) for more than 3 sets a day. Singing a song is also effective. Lung
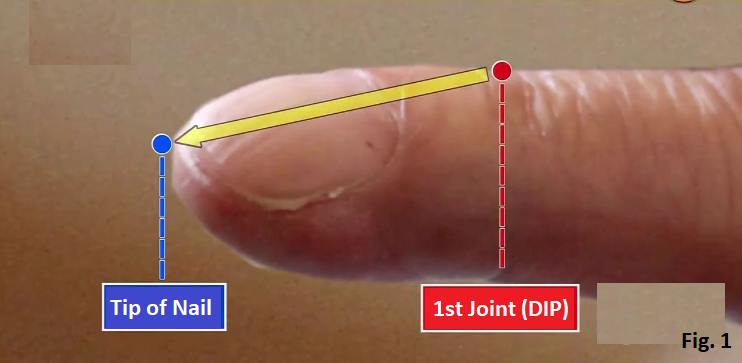
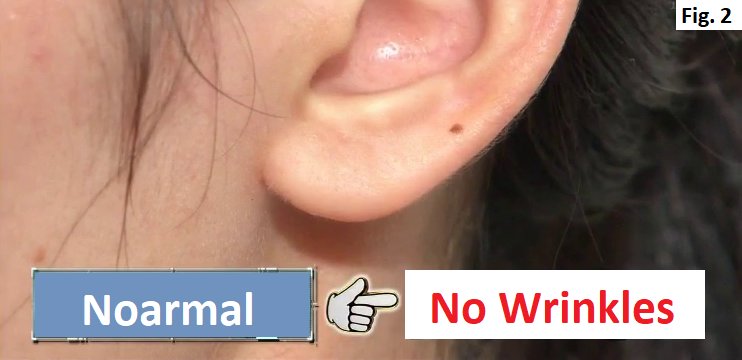
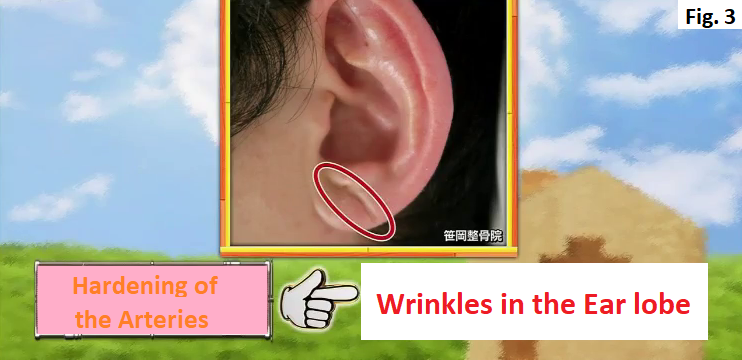
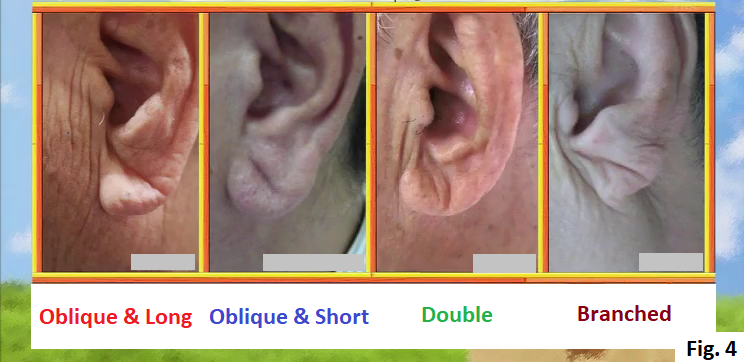
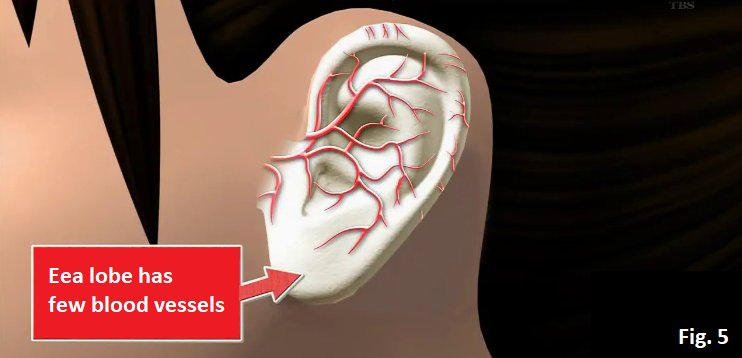
The sign of lung diseases shows up at the tip of the index finger. When you straighten the index finger horizontally, if the tip of the nail is lower than the first joint from the tip of the finger (Distal Interphalangeal Joint (DIP)), there is a high possibility of having lung diseases (Fig. 1). Hardening of the arteries (arteriosclerosis) Hardening of the arteries is the condition, which is caused by unhealthy lifestyle such as lack of exercise, unbalanced diet and smoking, that LDL cholesterol attaches on the wall of the artery, narrowing the artery and stopping the blood flow. Leaving hardening of the arteries as it is, it leads to heart attack or stroke. But looking at the ear can distinguish whether you have hardening of the arteries or not. How to check whether to have hardening of the arteries by looking at the ear A Normal person’s ear doesn’t have any wrinkles (Fig. 2), but the ear of a person with hardening of the arteries has wrinkles in the ear lobe (Fig. 3). There are various types of wrinkles as shown in Fig. 4. According to a research in University of Chicago, within 376 people who had heart attack, 275 people (73 %) had wrinkles in the ear. Why do wrinkles appear in the ear? The ear lobe has few blood vessels (Fig. 5). Hardening of the arteries causes poor blood flow of all the body, nutrition is not delivered to the ear lobe and the fat in the ear withers, causing wrinkles. How to check whether to have hardening of the arteries in the brain (1) Hold your nose with your left hand (Fig. 6). (2) Hold your left ear with your right hand (Fig. 7). (3) Replace your left hand by your right hand (Fig. 8). (4) Repeat (1)-(3) for more than 10 times within 10 seconds. If you can’t do this more than 10 times within 10 seconds, there is a possibility that the blood vessels in your brain have hardening of the arteries. If you leave it as it is, there is also a risk of developing stroke. When the blood flow in the brain is poor due to hardening of the arteries, it is difficult to transmit the order from the brain and that makes difficult to do fine movements. If you can with training, you don’t need to worry because people with hardening of the arteries in the brain can’t do this no matter how many times they try. A 75 years old woman was living with her daughter, her son-in-law and grandchildren. One day sore throat and cough started but there was no fever. At that night, severe cough started while she was sleeping. She went to her family doctor the next day and she was diagnosed with a common cold and prescribed with medication for that. 5 days after she started to take the medication, her cough didn’t stop. 2 weeks after she was diagnosed with a common cold, while sleeping, suddenly she couldn’t almost breathe like something was clogged in the throat. She was found by her family right before she lost her life and was sent to an emergency room. 3 hours later, her breathing calmed down and her life was saved. After that, various tests were performed and the disease was identified.
Asthma Asthma is a disease that airway or bronchial tubes are abnormally contracted by some reasons. Acute symptoms such as cough or difficulty of breathing are caused and if the attack is severe, it leads to death. There are 2 types of asthma. (1) Atopic asthma: allergic reaction to pollen or dust contracts the air way. (2) Non-atopic asthma: the cause of the contraction of the airway is unknown. In her case, the cause of the asthma attack was considered as deterioration of common cold, but after multiple tests, the cause was not specified. Therefore, she was diagnosed with non-atopic asthma. She was told that she had to get along with the disease trying some medicines to control the asthma attack. She was pushed down into the depth of anxiety because it was not sure when she would be attacked by the severe asthma symptoms. She started to take the prescribed medication, but suffered from the asthma attack again not only while sleeping but also anytime in her daily life. She could only keep taking the medication and stay home being afraid of the asthma attack. One day she happed to meet a monk of her acquaintance and she was referred to the monk’s brother who was a specialist of respiratory diseases. 2 months after the first episode, she visited his hospital. The doctor expected 5 causes of asthma attack that medicine didn’t work at all: (1) Rhinitis (2) Acid reflux (3) Heart failure which causes accumulation of water in the lungs, causing asthma attack (4) Direct damage to the lungs such as cancer or COPD He excluded (1) to (4) by the examination. The remaining expected cause is (5) Side effect of medication In rare cases, some of the medications for high blood pressure or analgesic and antipyretic (antifebrile and pain killer) cause asthma symptoms as their side effects. But she was not using any other medications except the prescribed medication. So all the expected causes were denied. He kept probing his data for 30 years of experience and recalled a case of 20 years ago and asked her if she went to an eye doctor to treat glaucoma. She was using eye drops for glaucoma. In the description of the eye drops, asthma attack was specified as a side effect. She consulted her eye doctor and changed to eye drops which didn’t have asthma attack as a side effect and the asthma symptom disappeared. 2 diseases that the colors of phlegm specify Yellowish white phlegm: Chronic sinus infection Inflammation occurs in sinus and pas or nasal discharge is accumulated, causing stuffy nose or other various symptoms. The pus or nasal discharge goes into the lung, causing inflammation and comes out as phlegm. Phlegm without any problem is translucent and white. Even if there is no stuffy nose, there can be yellowish white phlegm. Translucent and a little greenish: Acid reflux The entrance to the stomach loosens by age or other reasons and stomach acid backflows causing inflammation of esophagus, resulting in the symptoms such as burning sensation in the chest. Acid reflux also causes the inflammation of bronchial tubes, causing cough and phlegm especially when waking up in the morning. She was 55 years old. It started with small cough with phlegm. She judged it as a summer cold and took some over counter medicine and didn’t go see a doctor. She was confident about her health because she had been a nurse for 30 years and had just quit it. A week later small cough changed to strong cough. She woke up with strong cough and couldn’t sleep. She felt something wrong and went to a respiratory specialist and she was diagnosed as Pulmonary Mycobacterium Avium Complex (MAC) infection, which is a disease that Mycobacerium Avium Complex (MAC) goes into lungs by breathing and destroys lungs’ cells, leading to lowering of breathing function. Serious cases cause respiratory failure and in the worst case, it results in death. Recently this disease increases rapidly. What makes this disease dreadful is that it is impossible to specify the source of infection because MAC lives anywhere in soil and water so it is possible to infect MAC from a place where water is used such as shower or a bathtub and from gardening or playing with dirt. It means that it can happen to anyone at anytime and anywhere. Also once it occurs, it is difficult to cure and sometimes it is necessary to continue treatments throughout their lives. In her case, the symptom subsided after 2 years of medication. How to distinguish Summer-type Hypersensitivity Pneumonitis and Pulmonary MAC infection from a summer coldA summer cold is caused by viruses and usually subsides within 7-10 days. If the symptoms such as slight fever, cough or phlegm continue for more than 2 weeks, it is possible that it is no longer a summer cold.
She was 56 years old. It started with small cough. She went to see a doctor and was diagnosed as a summer cold. But one month later, it changed to heavy and strong cough. Also she started to feel difficulty of breathing and shortness of breath so that it became difficult to climb up stairs. Her husband and son started coughing as well. But their condition started getting better soon, but her condition got worse. There were differences about the condition among family members.
Then she went to a respiratory specialist and was diagnosed as Summer-type Hypersensitivity Pneumonitis, which is a type of pneumonitis that occurs as an allergic reaction caused by breathing in a substance of 1/300 mm increasing in summer. If the inflammation is repeated and it becomes chronic pneumonitis, the cells in lungs are gradually destroyed, resulting in disabling you for taking in oxygen. In the worst case, respiratory failure leads to death. Even if death is avoided, the destroyed cells in lungs won’t be recovered so you will possibly need ventilator throughout your life. The substance causing Summer-type Hypersensitivity Pneumonitis is something possible to appear in all houses in the coming season. That is Trichosporon which is a type of molds, and likes dampness and increases somewhere woods are used. In the case of the above woman, the floor of the bathroom rotted because a water pipe under the floor was leaking. Since the color of trichosporon is white or yellow so it is not noticeable, it increases at places where water is used such as a bathroom or a kitchen and also increases in a bed absorbing sweat. In the case of the above family, all three of them had Summer-type Hypersensitivity Pneumonitis. Her husband and son had mild symptoms because they went out for work and were not at home for a long time, but she had severe symptoms because she stayed home for a long time. After the renovation of the bathroom, her condition was improved. |
IchiroThis Blog is for a memo of my clinical realizations, information about health I have learned recently and update information. Archives
April 2024
Categories
All
|







 RSS Feed
RSS Feed